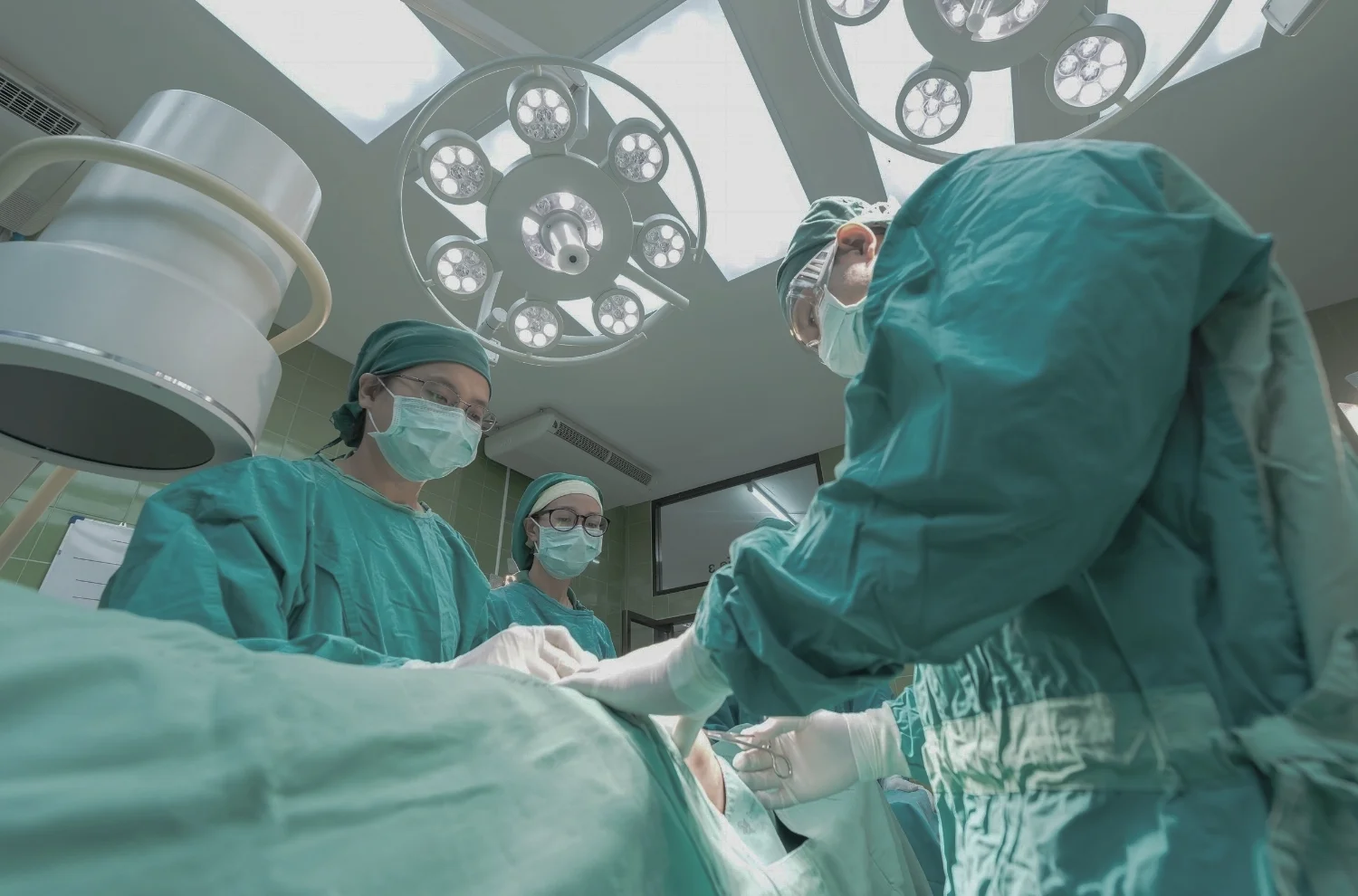
REASONS TO RETAIN A PATIENT ADVOCATE WHEN YOU FACE A SERIOUS ILLNESS
"Based on my own personal experience, it is so helpful not just to have a member of the family who is a physician but you can have a friend as well.
It doesn’t have to be a terminal illness. You can be going through something that is befuddling to you.
I’ve often used the phrase that most patients go into a doctor’s office as if it’s a Mayan temple and they don’t speak the language and whatever the doctor says they absorb…
What I’ve been recommending to my friends who are going through long-term serious illnesses—not necessarily cancer— you need a friend who is a physician off to the side. So that physician can become—man or woman—your interpreter and someone who can do independent research for you."
Tom Brokaw, NBC News Anchor and cancer patient since 2013
An Evening with Tom and Jennifer Brokaw
Chautauqua Institution, August 27, 2015
“A medical advocate is an independent physician who will do the things for you that doctors do for their loved ones when there is a serious health problem.”
It’s not easy for patients to deal with the healthcare system on their own when they learn they have a serious illness. Choices have to be made under the most difficult circumstances.
As a prominent physician put it after learning she had a malignant brain tumor, “It’s horrible, it’s shocking. It takes awhile to digest what’s happening.” But before long, she began combing through the latest medical literature, talking to experts and doing what physicians do for themselves and their families when a serious illness strikes. (1)
Most patients have no physician in their family to play that role. They and their families are on their own. To safeguard their care, they have to (1) educate themselves about alternative approaches to their problems and the risks and benefits of those alternatives; (2) identify a physician and hospital with an appropriate level of experience for providing needed diagnostic and therapeutic services; and (3) effectively communicate key medical information and personal preferences in short periods of contact with a physician.
“Many patients, doctors, nurses and health care leaders are concerned that the health care delivered is not, essentially, the care we should receive. ”
Patients who are unable to do those things may fall prey to “the serious quality gap” described below by the National Academy of Sciences’ Institute of Medicine. One option is to retain a medical advocate.
A medical advocate is an independent physician who will do the things for you that doctors do for their loved ones when there is a serious health problem, including researching alternatives, identifyingexpert physicians, preventing critical breakdowns in communication and coping with realities like these:
- "Many patients, doctors, nurses and health care leaders are concerned that the health care delivered is not, essentially, the care we should receive. The frustration levels of both patients and clinicians have probably never been higher. Yet the problems remain. Health care today harms too frequently and routinely fails to deliver its potential benefits.”
Those are not the words of a political activist group. They are the words of the Institute of Medicine, the health arm of the National Academy of Sciences. The IOM is an independent, nonprofit organization which works outside of government “to provide unbiased and authoritative advice to decision makers and the public.”
In its 2001 report, Crossing the Chasm: A New Health System for the 21st Century, the IOM also declared, “The prevailing model of health care delivery is complicated, comprising layers of processes and handoffs that patients and families find bewildering and clinicians view as wasteful. Patients in a 1996 Picker Survey reported that the health care system is a 'nightmare to navigate' that it feels less like a system than a confusing, expensive, unreliable, and often impersonal disarray.
“In sum, health care is plagued today by a serious quality gap. The current health care delivery system is not robust enough to apply medical knowledge and technology consistently in ways that are safe, effective, patient-centered, timely, efficient and equitable.” (9)
- Consider the sheer complexity of modern healthcare and the danger that creates for patients. Kenneth Kizer, M.D., M.P.H. is an expert on that subject. He has been repeatedly selected as one of the “100 Most Powerful People in Healthcare” by the magazine, Modern Healthcare. In the 1990’s, Dr. Kizer was the driving force behind a transformation of VA healthcare. He went on to serve as the founding President and CEO of the National Quality Forum where he developed a unique partnership of 300 organizations representing all parts of the healthcare industry.
Here then is how Dr. Kizer described the danger of medical errors: “The fact that errors occur in the delivery of healthcare should not be surprising, given the complexity of healthcare today. Indeed, modern healthcare is probably the most complex activity ever undertaken by human beings.”
“Relying on myriad highly complicated technologies, a panoply of powerful drugs and teams of caregivers who have widely differing professional backgrounds and who often operate with unclear lines of authority, healthcare is provided in highly variable physical settings and all of this typically occurs in a time-pressured highly stressed environment. Clearly, the circumstances prevalent in modern healthcare create an environment prone to error.” (3)
- Consider also that physicians face “an exploding knowledge base.” (3) This learning challenge is greater by far than what you find in other professions and it has given rise to “a gap between what we know works and what is actually done.” (4) Recent studies suggest that in the US, "adults receive 55% and children receive 47% of recommended therapies." (5)
- Next, consider the “volume-outcome conundrum.” As explained by Dr. Kizer, “There is considerable evidence that patients undergoing various types of complex treatments or high risk surgical procedures have lower mortality rates and otherwise better outcomes if care is provided in hospitals that have a high caseload of patients with the same condition than if care is provided by institutions with low caseloads of such patients... this relation between high volume and better outcome is strong and persistent, with approximately 300 studies on the subject..." (6)
- Finally, consider Dr. Jerome Groopman’s observation, “Usually doctors are right, but conservatively about 15 percent of all people are misdiagnosed. Some experts think it’s as high as 20 to 25 percent. And in half of those cases, there is serious injury or even death to the patient.”
“Usually doctors are right, but conservatively about 15 percent of all people are misdiagnosed. Some experts think it’s as high as 20 to 25 percent. And in half of those cases, there is serious injury or even death to the patient.”
Dr. Groopman is a professor at Harvard Medical School and author of the book, How Doctors Think. He says doctors’ diagnoses are wrong that often because “it’s very hard to be a doctor. We’re working under tremendous time pressure, especially in the current medical system. But the reasons we are wrong are not related to technical mistakes, like someone putting the wrong name on an X-ray or mixing up a blood specimen in the lab. Nor is it really ignorance about what the actual disease is. We make misdiagnoses because we make errors in thinking.” (7)
The most important advice that Dr. Groopman gives to patients is “to keep asking questions; to not give up even if their physician has apparently given up; to empathize with time demands imposed on physicians; and to be honest with their physician, even if it means communicating their unease with their physician’s approach to their disease.” (8)
1. Cohen E. After cancer diagnosis, what comes next? CNN.com. May 21, 2008. http://cnn.com/2008/HEALTH/conditions/05/21/ep.cancer.resources/index.html.
2. Kizer KW. Patient Safety: A Call to Action: A Consensus Statement from the National Quality Forum. Medscape Gen Med. 2001;3(1).
3. Kizer KW. Putting the Ideas into Practice. Medical Care. 2003;41:I-87.
4. McGlynn EA et al. The quality of healthcare delivered to adults in the United States. N Eng J Med. 2003;348:2635.
5. Matthews SC. Physician Autonomy and Informed Decision Making Finding the Balance for Patient Safety and Quality. JAMA. 2008;300:2913.
6. Kizer KW. The Volume-Outcome Conundrum. N Eng J Med. 2003;349:2159.
7. Groopman: The Doctor’s In, But Is He Listening? Interview of Jerome Groopman, NPR Morning Edition.
March 16, 2007.
8. Wang-Gillam A. How Doctors Think. JAMA. 2007;298:688.
9.Institute of Medicine. Crossing the Quality Chasm. A New Health System for the 21st Century. National Academy Press, 2001.